The Sleeve Gastrectomy is a purely restrictive procedure, whereby it limits the amount of food that can be eaten at one time. For some patients the gastric sleeve is the first part of a two part surgical procedure. Like all weight loss surgeries, the gastric sleeve requires that patients follow a healthy diet and incorporate an exercise plan into their lifestyle in order to continue and then sustain weight loss.
The Procedure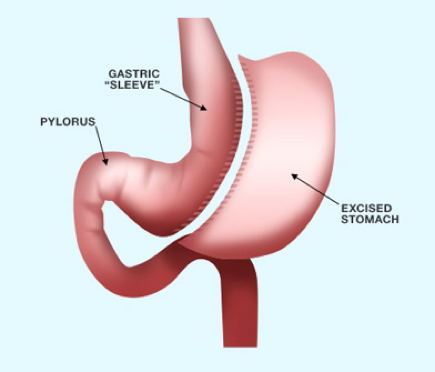
The gastric sleeve procedure (also known as a vertical sleeve gastrectomy) involves removing two-thirds of the left side of the stomach. The stomach is reduced surgically by approximately 80% creating a gastric “sleeve.” No changes are made to the remainder of the intestines which allows for normal digestion and absorption. Ghrelin producing cells are reduced with the removal of a portion of the stomach thus diminishing the sensation of hunger.
Advantages and Results
- Patients can expect to loss 70% of their excess weight at the end of one year.
- Weight loss begins immediately.
- The major part of the stomach that produces hormone responsible for stimulating hunger is removed thus reducing the sensation of hunger. Patient often feel less hungry and state the desire to eat is reduced.
- Does not require implanting an artificial device in the abdomen.
- Does not require manipulation as with the adjustable gastric band.
- Far fewer restrictions are required on the foods that patients can eat following surgery, as compared to other bypass procedures, because the stomach continues to function normally.
- Patients are not at greater risk for complications such as intestinal obstruction, anemia or vitamin deficiencies.
Possible Complications
The various possible complications associated with the sleeve gastrectomy are listed below. It would be best to talk about these and other potential complications with your physician.
- Leaks can occur and may be from staple lines or due to poor healing.
- Marginal ulcers – ulcers in the gastric sleeve that can bleed, perforate (create a hole in the gastric pouch) or heal and cause narrowing of the gastric sleeve.
- Strictures or narrowing of the gastric sleeve. This can occur due to scar tissue or ulcer disease.
- Obstructions can occur due to scar tissue or ulcer disease.
- Vitamin and mineral deficiency can occur therefore patients are encouraged to take vitamin supplementation. It is recommended that all patients have their vitamin levels checked at regular intervals.
- Hernias can develop in up to 10 to 20 percent of patients after any type of abdominal surgery.
- Gallstones can occur due to rapid weight loss.
- Intolerance to certain foods can occur. It is recommended that patients speak with their surgeon or a registered dietitian if they are experiencing this.
- Stretching and enlargement of the gastric sleeve can occur over time. This can lead to weight gain.
- Weight gain can occur if patients do not comply with the appropriate dietary guidelines. It is recommended that all patients follow up at regular intervals during the first year and yearly thereafter with their bariatric surgeon. The best prevention to weight gain is early identification of maladaptive behaviors and modifying them.
- Due to the nature of this procedure it is not reversible.
Sources: Medline Plus (National Institutes of Health), American Society for Metabolic & Bariatric Surgery
